New publication: disease burden of myotonic dystrophy type 1
Nikoletta Nikolenko and Erik Landfeldt have published a new study on the impact of myotonic dystrophy type 1 (DM1) in the Journal of Neurology. They use a questionnaire-based method, the Individualized Neuromuscular Quality of Life Questionnaire (INQoL), to assess the burden of this condition on affected adults. The study provides further evidence of the wide range of domains affected in this multisystem disease. They are also able to show that INQoL scores correlate with the severity of the underlying genetic defect, linking CTG expansion with burden of illness. The study provides important baseline data for healthcare and for clinical research in myotonic dystrophy.
The full publication is available to read at the journal’s website here (open access)
Disease burden of myotonic dystrophy type 1
Landfeldt, E., Nikolenko, N., Jimenez-Moreno, C. Cumming, S., Monckton, D.G., Gorman, G., Turner, C.,Lochmüller, H.
J Neurol (2019).
https://doi.org/10.1007/s00415-019-09228-w
Abstract
Objective
The objective of this cross-sectional, observational study was to investigate the disease burden of myotonic dystrophy type 1 (DM1), a disabling muscle disorder.
Methods
Adults with DM1 were recruited as part of the PhenoDM1 study from Newcastle University (Newcastle upon Tyne, UK). Disease burden data were recorded through the Individualized Neuromuscular Quality of Life (INQoL) questionnaire. Results were examined by sex and clinical variables [e.g. the six-minute walk test (6MWT), the Mini Mental State Examination, and estimated progenitor and modal allele CTG repeat length].
Results
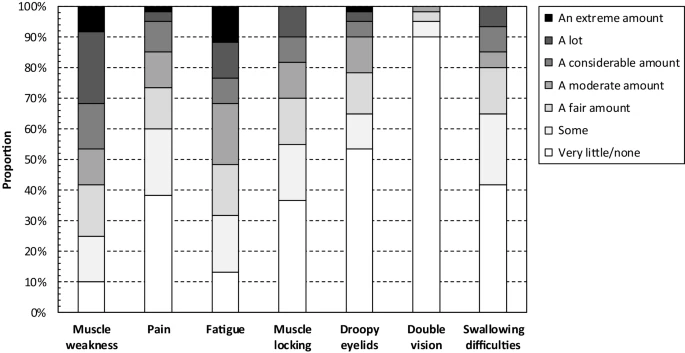
Our sample consisted of 60 patients with DM1 (mean age: 45 years; 45% female). Muscle weakness and fatigue constituted the two most common disease manifestations, reported by 93% and 90% of patients, respectively, followed by muscle locking (73%). Most patients (> 55%) reported feeling anxious/worried, depressed, frustrated, and/or having low confidence/self-esteem, 23% and 33% indicated substantial impairment of daily and leisure activities, respectively, and 47% did not work as a consequence of the disease. Estimated progenitor CTG length corrected by age correlated surprisingly well with INQoL scores. Differences by sex were generally minor.
Conclusion
We show that DM1 is associated with a substantial disease burden resulting in impairment across many different domains of patients’ lives, emphasizing the need for a holistic approach to medical management. Our results also show that the INQoL records relevant information about patients with DM1, but that further investigation of the psychometric properties of the scale is needed for meaningful interpretation of instrument scores.