New Publication: Salbutamol modifies the neuromuscular junction in a mouse model of ColQ myasthenic syndrome
While we know some drug treatments can help patients with disruption of the neuromuscular junction (NMJ) we do not always know why they work. Determining the mechanism or indeed mechanisms of action of a successful treatment may help us develop even more effective drugs though increasing specificity or reducing side effects. Here we show that one site of action of the β-adrenergic agonist salbutamol is the postsynaptic junction and the NMJ itself. Furthermore the improvements in muscle strength occurred in the absence of significant changes in muscle fibre size.

Article author Grace McMacken.
Read the full open access publication here.
Abstract
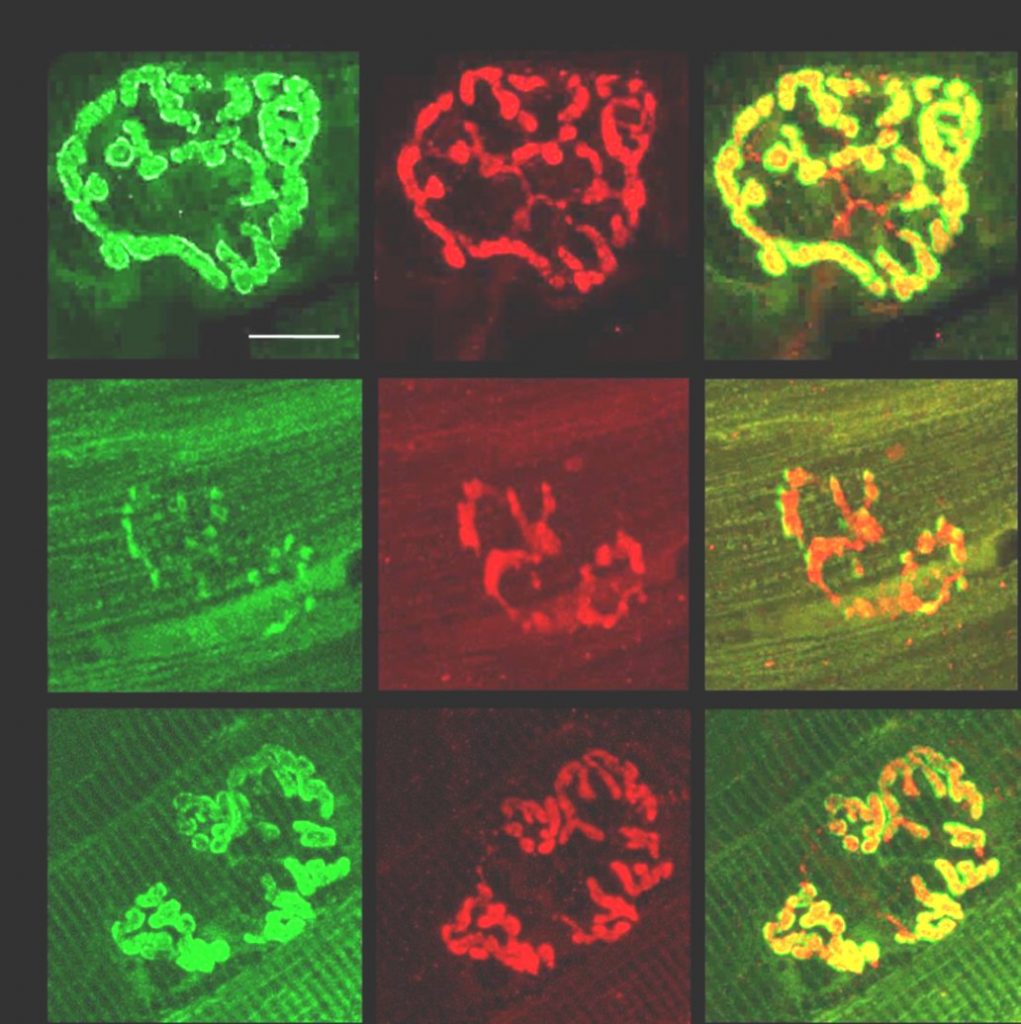
The β-adrenergic agonists salbutamol and ephedrine have proven to be effective as therapies for human disorders of the neuromuscular junction, in particular many subsets of congenital myasthenic syndromes. However, the mechanisms underlying this clinical benefit are unknown and improved understanding of the effect of adrenergic signalling on the neuromuscular junction is essential to facilitate the development of more targeted therapies. Here, we investigated the effect of salbutamol treatment on the NMJ in the ColQ deficient mouse, a model of end-plate acetylcholinesterase deficiency. ColQ-/- mice received 7 weeks of daily salbutamol injection, and the effect on muscle strength and neuromuscular junction morphology was analysed. We show that salbutamol leads to a gradual improvement in muscle strength in ColQ-/- mice. In addition, the neuromuscular junctions of salbutamol treated mice showed significant improvements in several postsynaptic morphological defects, including increased synaptic area, acetylcholine receptor area and density, and extent of postjunctional folds. These changes occurred without alterations in skeletal muscle fibre size or type. These findings suggest that β-adrenergic agonists lead to functional benefit in the ColQ-/- mouse and to long-term structural changes at the neuromuscular junction. These effects are primarily at the postsynaptic membrane and may lead to enhanced neuromuscular transmission.